Details of Drug-Drug Interaction
| Drug General Information (ID: DDIVSGAH0K) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Drug Name | Thiethylperazine | Drug Info | Safinamide | Drug Info | |||||
| Drug Type | Small molecule | Small molecule | |||||||
| Therapeutic Class | Antiemetics | Dopaminergic Antiparkinsonism Agents | |||||||
| Structure | |||||||||
| Mechanism of Thiethylperazine-Safinamide Interaction (Severity Level: Moderate) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
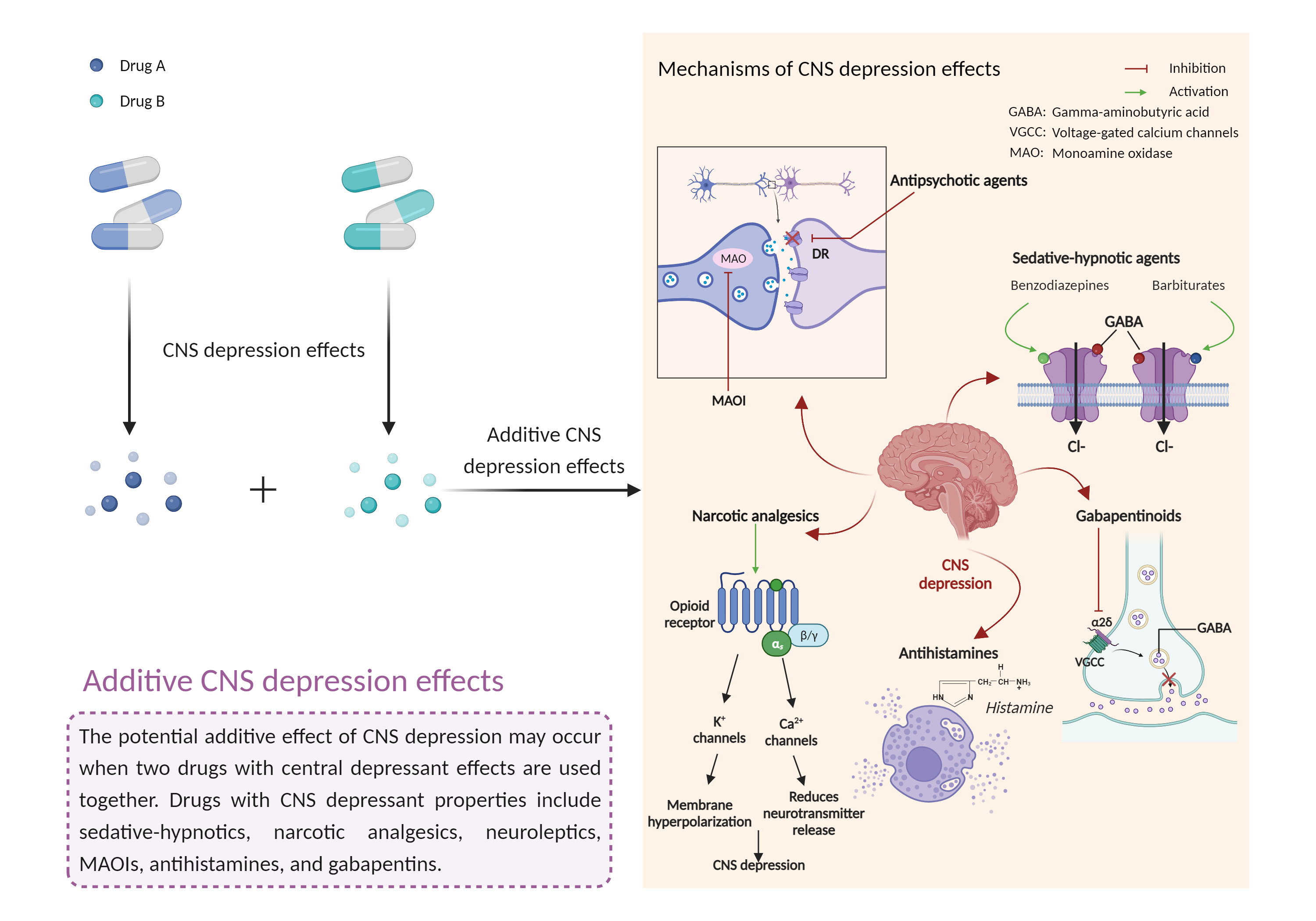
| Additive CNS depression effects Click to Show/Hide Mechanism Graph | |||||||||
 |
|||||||||
| Drug Name | Thiethylperazine | Safinamide | |||||||
| Mechanism 1 | CNS depression effects | CNS depression effects | |||||||
| Key Mechanism Factor 1 | |||||||||
| Factor Name | CNS depression effects | ||||||||
| Factor Description | CNS depressants are drugs that inhibit or suppress brain activity and can reduce mental and physical processes. Excessive CNS depression can lead to decreased heart rate, slow breathing (less than 10 breaths per minute), extreme confusion or loss of memory, nausea and vomiting, poor judgment, blue lips or fingertips, irritability and aggression, and clammy or cold skin. | ||||||||
| Mechanism Description |
|
||||||||
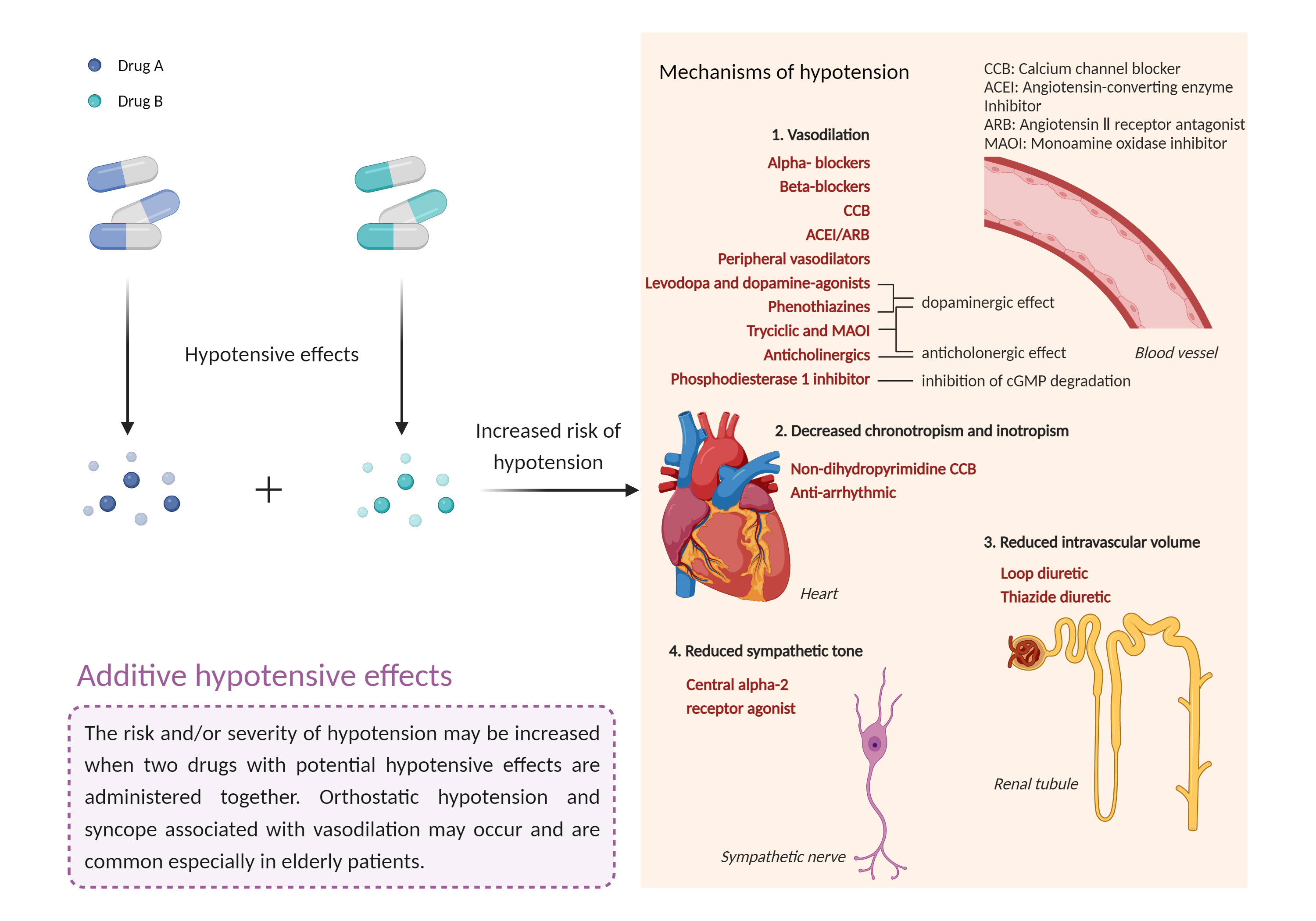
| Additive hypotensive effects Click to Show/Hide Mechanism Graph | |||||||||
 |
|||||||||
| Drug Name | Thiethylperazine | Safinamide | |||||||
| Mechanism 2 |
Hypotensive effects Alpha-1 adrenergic receptor Antagonist |
Hypotensive effects Monoamine oxidase-B selective Inhibitor |
|||||||
| Key Mechanism Factor 2 | |||||||||
| Factor Name | Adrenergic receptor alpha-1 | Structure Sequence | |||||||
| Protein Family | G-protein coupled receptor 1 family | ||||||||
| Protein Function |
This alpha-adrenergic receptor mediates its action by association with G proteins that activate a phosphatidylinositol-calcium second messenger system. Its effect is mediated by G(q) and G(11) proteins. Nuclear ADRA1A-ADRA1B heterooligomers regulate phenylephrine(PE)-stimulated ERK signaling in cardiac myocytes.
Click to Show/Hide
|
||||||||
| Key Mechanism Factor 3 | |||||||||
| Factor Name | Monoamine oxidase type B |
×
Structure
Sequence
MSNKCDVVVVGGGISGMAAAKLLHDSGLNVVVLEARDRVGGRTYTLRNQKVKYVDLGGSYVGPTQNRILRLAKELGLETYKVNEVERLIHHVKGKSYPFRGPFPPVWNPITYLDHNNFWRTMDDMGREIPSDAPWKAPLAEEWDNMTMKELLDKLCWTESAKQLATLFVNLCVTAETHEVSALWFLWYVKQCGGTTRIISTTNGGQERKFVGGSGQVSERIMDLLGDRVKLERPVIYIDQTRENVLVETLNHEMYEAKYVISAIPPTLGMKIHFNPPLPMMRNQMITRVPLGSVIKCIVYYKEPFWRKKDYCGTMIIDGEEAPVAYTLDDTKPEGNYAAIMGFILAHKARKLARLTKEERLKKLCELYAKVLGSLEALEPVHYEEKNWCEEQYSGGCYTTYFPPGILTQYGRVLRQPVDRIYFAGTETATHWSGYMEGAVEAGERAAREILHAMGKIPEDEIWQSEPESVDVPAQPITTTFLERHLPSVPGLLRLIGLTTIFSATALGFLAHKRGLLVRV
|
|||||||
| Gene Name | MAOB | ||||||||
| Uniprot ID | AOFB_HUMAN | ||||||||
| KEGG Pathway | hsa:4129 | ||||||||
| Protein Family | Flavin monoamine oxidase family | ||||||||
| Protein Function |
Catalyzes the oxidative deamination of primary and some secondary amines such as neurotransmitters, and exogenous amines including the tertiary amine, neurotoxin 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP), with concomitant reduction of oxygen to hydrogen peroxide and participates in the metabolism of neuroactive and vasoactive amines in the central nervous system and peripheral tissues (PubMed:11134050, PubMed:8665924, PubMed:8316221, PubMed:11049757, PubMed:20493079). Preferentially degrades benzylamine and phenylethylamine (PubMed:11134050, PubMed:8665924, PubMed:8316221, PubMed:11049757, PubMed:20493079).
Click to Show/Hide
|
||||||||
| Mechanism Description |
|
||||||||
| Recommended Action | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Management | Although often safe and effective, caution is advised during coadministration of MAOIs and phenothiazines, especially during the first few weeks of treatment. Close monitoring for development of hypotension is recommended. Patients should be advised to avoid rising abruptly from a sitting or recumbent position and to notify their physician if they experience dizziness, lightheadedness, syncope, orthostasis, or tachycardia. Ambulatory patients should also be counseled to avoid hazardous activities requiring mental alertness and motor coordination until they know how these agents affect them, and to notify their physician if they experience excessive or prolonged CNS effects that interfere with their normal activities. Alcohol should be avoided, since it may increase hypotensive and CNS effects. | ||||||||
