Details of Drug-Drug Interaction
| Drug General Information (ID: DDILQE8XN5) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Drug Name | Sulfasalazine | Drug Info | Anisindione | Drug Info | |||||
| Drug Type | Small molecule | Small molecule | |||||||
| Therapeutic Class | Antiinflammatory Agents | Anticoagulants | |||||||
| Structure | |||||||||
| Mechanism of Sulfasalazine-Anisindione Interaction (Severity Level: Major) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
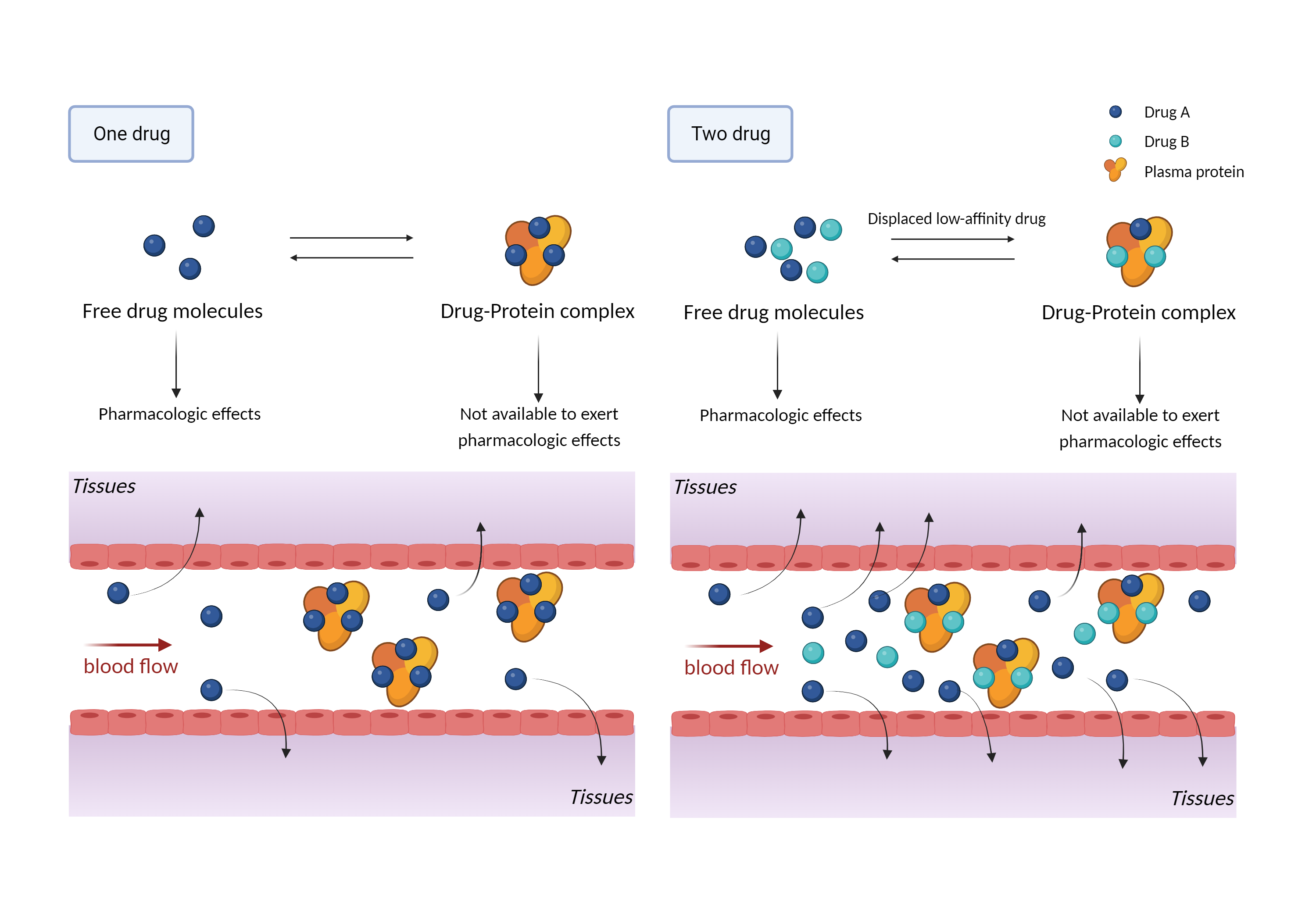
| Competitive binding of plasma proteins Click to Show/Hide Mechanism Graph | |||||||||
 |
|||||||||
| Drug Name | Sulfasalazine | Anisindione | |||||||
| Mechanism 1 | Competition for plasma protein binding sites | Competition for plasma protein binding sites | |||||||
| Key Mechanism Factor 1 | |||||||||
| Factor Name | Plasma protein binding | ||||||||
| Factor Description | Plasma protein binding refers to the degree of binding of a drug to proteins in the blood, and the lower the degree of binding, the more efficiently the drug can cross cell membranes or diffuse. Plasma protein binding alters the distribution and therapeutic characteristics of the drugs. | ||||||||
| Mechanism Description |
|
||||||||
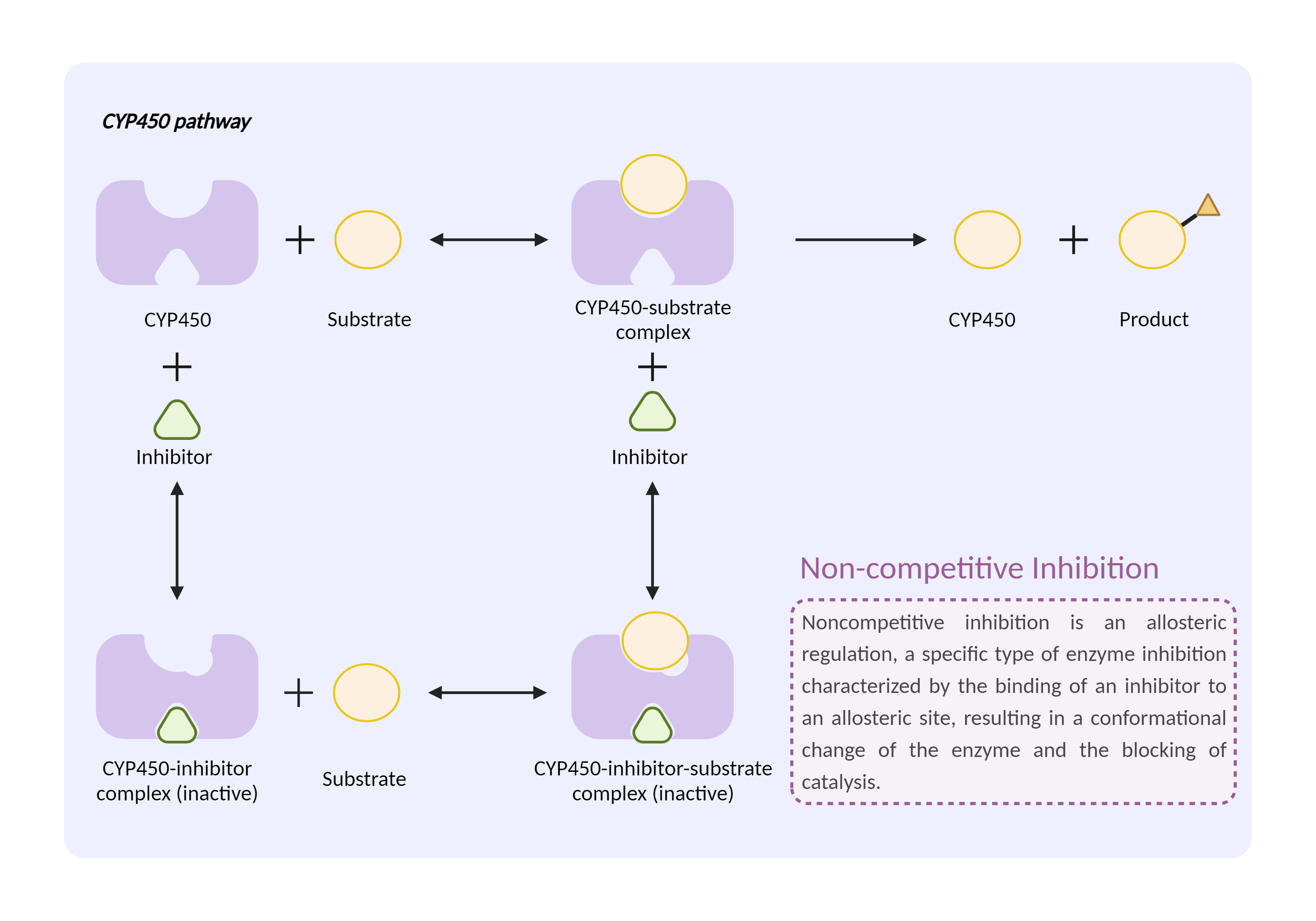
| CYP450 enzyme inhibition Click to Show/Hide Mechanism Graph | |||||||||
 |
|||||||||
| Drug Name | Sulfasalazine | Anisindione | |||||||
| Mechanism 2 | CYP450 2C9 inhibitor | CYP450 2C9 substrate | |||||||
| Key Mechanism Factor 2 | |||||||||
| Factor Name | Cytochrome P450 2C9 |
×
Structure
Sequence
MDSLVVLVLCLSCLLLLSLWRQSSGRGKLPPGPTPLPVIGNILQIGIKDISKSLTNLSKVYGPVFTLYFGLKPIVVLHGYEAVKEALIDLGEEFSGRGIFPLAERANRGFGIVFSNGKKWKEIRRFSLMTLRNFGMGKRSIEDRVQEEARCLVEELRKTKASPCDPTFILGCAPCNVICSIIFHKRFDYKDQQFLNLMEKLNENIKILSSPWIQICNNFSPIIDYFPGTHNKLLKNVAFMKSYILEKVKEHQESMDMNNPQDFIDCFLMKMEKEKHNQPSEFTIESLENTAVDLFGAGTETTSTTLRYALLLLLKHPEVTAKVQEEIERVIGRNRSPCMQDRSHMPYTDAVVHEVQRYIDLLPTSLPHAVTCDIKFRNYLIPKGTTILISLTSVLHDNKEFPNPEMFDPHHFLDEGGNFKKSKYFMPFSAGKRICVGEALAGMELFLFLTSILQNFNLKSLVDPKNLDTTPVVNGFASVPPFYQLCFIPV
|
|||||||
| Gene Name | CYP2C9 | ||||||||
| Uniprot ID | CP2C9_HUMAN | ||||||||
| KEGG Pathway | hsa:1559 | ||||||||
| Protein Family | Cytochrome P450 family | ||||||||
| Protein Function |
A cytochrome P450 monooxygenase involved in the metabolism of various endogenous substrates, including fatty acids and steroids (PubMed:7574697, PubMed:9866708, PubMed:9435160, PubMed:12865317, PubMed:15766564, PubMed:19965576, PubMed:21576599). Mechanistically, uses molecular oxygen inserting one oxygen atom into a substrate, and reducing the second into a water molecule, with two electrons provided by NADPH via cytochrome P450 reductase (NADPH--hemoprotein reductase) (PubMed:7574697, PubMed:9866708, PubMed:9435160, PubMed:12865317, PubMed:15766564, PubMed:19965576, PubMed:21576599). Catalyzes the epoxidation of double bonds of polyunsaturated fatty acids (PUFA) (PubMed:7574697, PubMed:15766564, PubMed:19965576, PubMed:9866708). Catalyzes the hydroxylation of carbon-hydrogen bonds. Metabolizes cholesterol toward 25-hydroxycholesterol, a physiological regulator of cellular cholesterol homeostasis (PubMed:21576599). Exhibits low catalytic activity for the formation of catechol estrogens from 17beta-estradiol (E2) and estrone (E1), namely 2-hydroxy E1 and E2 (PubMed:12865317). Catalyzes bisallylic hydroxylation and hydroxylation with double-bond migration of polyunsaturated fatty acids (PUFA) (PubMed:9866708, PubMed:9435160). Also metabolizes plant monoterpenes such as limonene. Oxygenates (R)- and (S)-limonene to produce carveol and perillyl alcohol (PubMed:11950794). Contributes to the wide pharmacokinetics variability of the metabolism of drugs such as S-warfarin, diclofenac, phenytoin, tolbutamide and losartan (PubMed:25994031).
Click to Show/Hide
|
||||||||
| Mechanism Description |
|
||||||||
| Recommended Action | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Management | Patients receiving coumarin anticoagulants should be closely monitored during concomitant therapy with sulfonamides. The INR should be checked frequently and coumarin dosage adjusted accordingly, particularly following initiation or discontinuation of sulfonamide therapy in patients who are stabilized on their anticoagulant regimen. The same precaution may be applicable during therapy with other oral anticoagulants (e.g., indandiones), although clinical data are lacking. Patients should be advised to promptly report any signs of bleeding to their physician, including pain, swelling, headache, dizziness, weakness, prolonged bleeding from cuts, increased menstrual flow, vaginal bleeding, nosebleeds, bleeding of gums from brushing, unusual bleeding or bruising, red or brown urine, or red or black stools. | ||||||||
