Details of Drug-Drug Interaction
| Drug General Information (ID: DDI52WXL7B) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Drug Name | Trandolapril | Drug Info | Indapamide | Drug Info | |||||
| Drug Type | Small molecule | Small molecule | |||||||
| Therapeutic Class | Antihypertensive Agents | Antihypertensive Agents | |||||||
| Structure | |||||||||
| Mechanism of Trandolapril-Indapamide Interaction (Severity Level: Moderate) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Additive hypotensive effects Click to Show/Hide Mechanism Graph | |||||||||
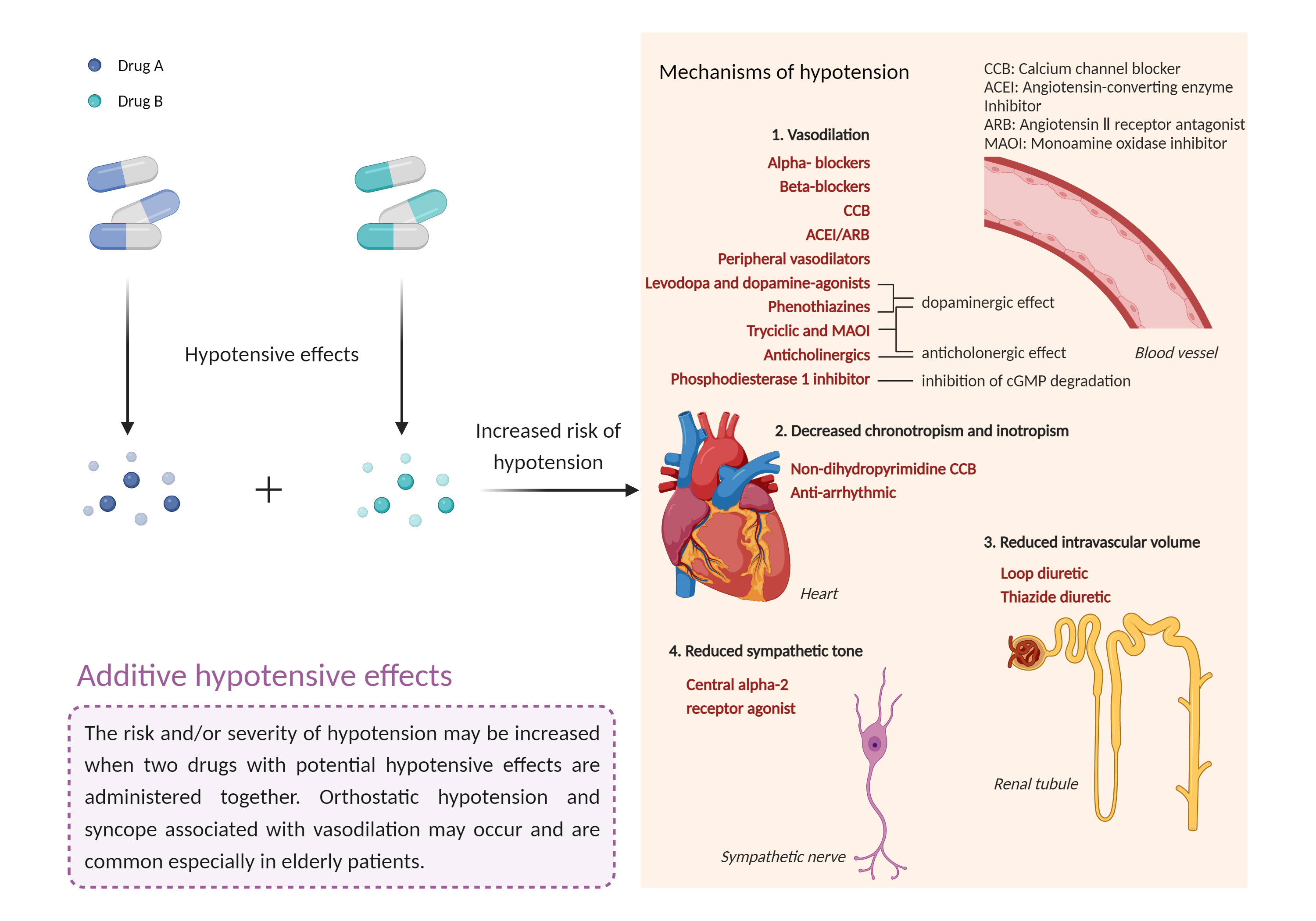 |
|||||||||
| Drug Name | Trandolapril | Indapamide | |||||||
| Mechanism |
Antihypertensive agent Angiotensin-converting enzyme Inhibitor |
Hypotensive effects Voltage-gated potassium channel Blocker |
|||||||
| Key Mechanism Factor 1 | |||||||||
| Factor Name | Angiotensin-converting enzyme |
×
Structure
Sequence
MGAASGRRGPGLLLPLPLLLLLPPQPALALDPGLQPGNFSADEAGAQLFAQSYNSSAEQVLFQSVAASWAHDTNITAENARRQEEAALLSQEFAEAWGQKAKELYEPIWQNFTDPQLRRIIGAVRTLGSANLPLAKRQQYNALLSNMSRIYSTAKVCLPNKTATCWSLDPDLTNILASSRSYAMLLFAWEGWHNAAGIPLKPLYEDFTALSNEAYKQDGFTDTGAYWRSWYNSPTFEDDLEHLYQQLEPLYLNLHAFVRRALHRRYGDRYINLRGPIPAHLLGDMWAQSWENIYDMVVPFPDKPNLDVTSTMLQQGWNATHMFRVAEEFFTSLELSPMPPEFWEGSMLEKPADGREVVCHASAWDFYNRKDFRIKQCTRVTMDQLSTVHHEMGHIQYYLQYKDLPVSLRRGANPGFHEAIGDVLALSVSTPEHLHKIGLLDRVTNDTESDINYLLKMALEKIAFLPFGYLVDQWRWGVFSGRTPPSRYNFDWWYLRTKYQGICPPVTRNETHFDAGAKFHVPNVTPYIRYFVSFVLQFQFHEALCKEAGYEGPLHQCDIYRSTKAGAKLRKVLQAGSSRPWQEVLKDMVGLDALDAQPLLKYFQPVTQWLQEQNQQNGEVLGWPEYQWHPPLPDNYPEGIDLVTDEAEASKFVEEYDRTSQVVWNEYAEANWNYNTNITTETSKILLQKNMQIANHTLKYGTQARKFDVNQLQNTTIKRIIKKVQDLERAALPAQELEEYNKILLDMETTYSVATVCHPNGSCLQLEPDLTNVMATSRKYEDLLWAWEGWRDKAGRAILQFYPKYVELINQAARLNGYVDAGDSWRSMYETPSLEQDLERLFQELQPLYLNLHAYVRRALHRHYGAQHINLEGPIPAHLLGNMWAQTWSNIYDLVVPFPSAPSMDTTEAMLKQGWTPRRMFKEADDFFTSLGLLPVPPEFWNKSMLEKPTDGREVVCHASAWDFYNGKDFRIKQCTTVNLEDLVVAHHEMGHIQYFMQYKDLPVALREGANPGFHEAIGDVLALSVSTPKHLHSLNLLSSEGGSDEHDINFLMKMALDKIAFIPFSYLVDQWRWRVFDGSITKENYNQEWWSLRLKYQGLCPPVPRTQGDFDPGAKFHIPSSVPYIRYFVSFIIQFQFHEALCQAAGHTGPLHKCDIYQSKEAGQRLATAMKLGFSRPWPEAMQLITGQPNMSASAMLSYFKPLLDWLRTENELHGEKLGWPQYNWTPNSARSEGPLPDSGRVSFLGLDLDAQQARVGQWLLLFLGIALLVATLGLSQRLFSIRHRSLHRHSHGPQFGSEVELRHS
|
|||||||
| Gene Name | ACE | ||||||||
| Uniprot ID | ACE_HUMAN | ||||||||
| KEGG Pathway | hsa:1636 | ||||||||
| Protein Family | Peptidase M2 family | ||||||||
| Protein Function |
Converts angiotensin I to angiotensin II by release of the terminal His-Leu, this results in an increase of the vasoconstrictor activity of angiotensin. Also able to inactivate bradykinin, a potent vasodilator. Has also a glycosidase activity which releases GPI-anchored proteins from the membrane by cleaving the mannose linkage in the GPI moiety.
Click to Show/Hide
|
||||||||
| Key Mechanism Factor 2 | |||||||||
| Factor Name | Voltage-gated potassium channel Kv7.1 |
×
Structure
Sequence
MAAASSPPRAERKRWGWGRLPGARRGSAGLAKKCPFSLELAEGGPAGGALYAPIAPGAPGPAPPASPAAPAAPPVASDLGPRPPVSLDPRVSIYSTRRPVLARTHVQGRVYNFLERPTGWKCFVYHFAVFLIVLVCLIFSVLSTIEQYAALATGTLFWMEIVLVVFFGTEYVVRLWSAGCRSKYVGLWGRLRFARKPISIIDLIVVVASMVVLCVGSKGQVFATSAIRGIRFLQILRMLHVDRQGGTWRLLGSVVFIHRQELITTLYIGFLGLIFSSYFVYLAEKDAVNESGRVEFGSYADALWWGVVTVTTIGYGDKVPQTWVGKTIASCFSVFAISFFALPAGILGSGFALKVQQKQRQKHFNRQIPAAASLIQTAWRCYAAENPDSSTWKIYIRKAPRSHTLLSPSPKPKKSVVVKKKKFKLDKDNGVTPGEKMLTVPHITCDPPEERRLDHFSVDGYDSSVRKSPTLLEVSMPHFMRTNSFAEDLDLEGETLLTPITHISQLREHHRATIKVIRRMQYFVAKKKFQQARKPYDVRDVIEQYSQGHLNLMVRIKELQRRLDQSIGKPSLFISVSEKSKDRGSNTIGARLNRVEDKVTQLDQRLALITDMLHQLLSLHGGSTPGSGGPPREGGAHITQPCGSGGSVDPELFLPSNTLPTYEQLTVPRRGPDEGS
|
|||||||
| Gene Name | KCNQ1 | ||||||||
| Uniprot ID | KCNQ1_HUMAN | ||||||||
| KEGG Pathway | hsa:3784 | ||||||||
| Protein Family | Potassium channel family | ||||||||
| Protein Function |
Potassium channel that plays an important role in a number of tissues, including heart, inner ear, stomach and colon (PubMed:10646604, PubMed:25441029). Associates with KCNE beta subunits that modulates current kinetics (PubMed:9312006, PubMed:9108097, PubMed:8900283, PubMed:10646604, PubMed:11101505, PubMed:19687231). Induces a voltage-dependent current by rapidly activating and slowly deactivating potassium-selective outward current (PubMed:9312006, PubMed:9108097, PubMed:8900283, PubMed:10646604, PubMed:11101505, PubMed:25441029). Promotes also a delayed voltage activated potassium current showing outward rectification characteristic (By similarity). During beta-adrenergic receptor stimulation participates in cardiac repolarization by associating with KCNE1 to form the I(Ks) cardiac potassium current that increases the amplitude and slows down the activation kinetics of outward potassium current I(Ks) (By similarity) (PubMed:9312006, PubMed:9108097, PubMed:8900283, PubMed:10646604, PubMed:11101505). Muscarinic agonist oxotremorine-M strongly suppresses KCNQ1/KCNE1 current (PubMed:10713961). When associated with KCNE3, forms the potassium channel that is important for cyclic AMP-stimulated intestinal secretion of chloride ions (PubMed:10646604). This interaction with KCNE3 is reduced by 17beta-estradiol, resulting in the reduction of currents (By similarity). During conditions of increased substrate load, maintains the driving force for proximal tubular and intestinal sodium ions absorption, gastric acid secretion, and cAMP-induced jejunal chloride ions secretion (By similarity). Allows the provision of potassium ions to the luminal membrane of the secretory canaliculus in the resting state as well as during stimulated acid secretion (By similarity). When associated with KCNE2, forms a heterooligomer complex leading to currents with an apparently instantaneous activation, a rapid deactivation process and a linear current-voltage relationship and decreases the amplitude of the outward current (PubMed:11101505). When associated with KCNE4, inhibits voltage-gated potassium channel activity (PubMed:19687231). When associated with KCNE5, this complex only conducts current upon strong and continued depolarization (PubMed:12324418). Also forms a heterotetramer with KCNQ5; has a voltage-gated potassium channel activity (PubMed:24855057). Binds with phosphatidylinositol 4,5-bisphosphate (PubMed:25037568).
Click to Show/Hide
|
||||||||
| Mechanism Description |
|
||||||||
| Recommended Action | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Management | Monitoring of blood pressure, diuresis, electrolytes, and renal function is recommended during coadministration. The possibility of first-dose hypotensive effects may be minimized by initiating therapy with small doses of the ACE inhibitor, or either discontinuing the diuretic temporarily or increasing the salt intake approximately one week prior to initiating an ACE inhibitor. alternatively, the patient may remain under medical supervision for at least two hours after the first dose of the ACE inhibitor, or until blood pressure has stabilized. | ||||||||
