Details of Drug-Drug Interaction
| Drug General Information (ID: DDI2ROUYPH) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Drug Name | Metyrosine | Drug Info | Canagliflozin | Drug Info | |||||
| Drug Type | Small molecule | Small molecule | |||||||
| Therapeutic Class | Antineoplastics | Antidiabetic Agents | |||||||
| Structure | |||||||||
| Mechanism of Metyrosine-Canagliflozin Interaction (Severity Level: Moderate) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
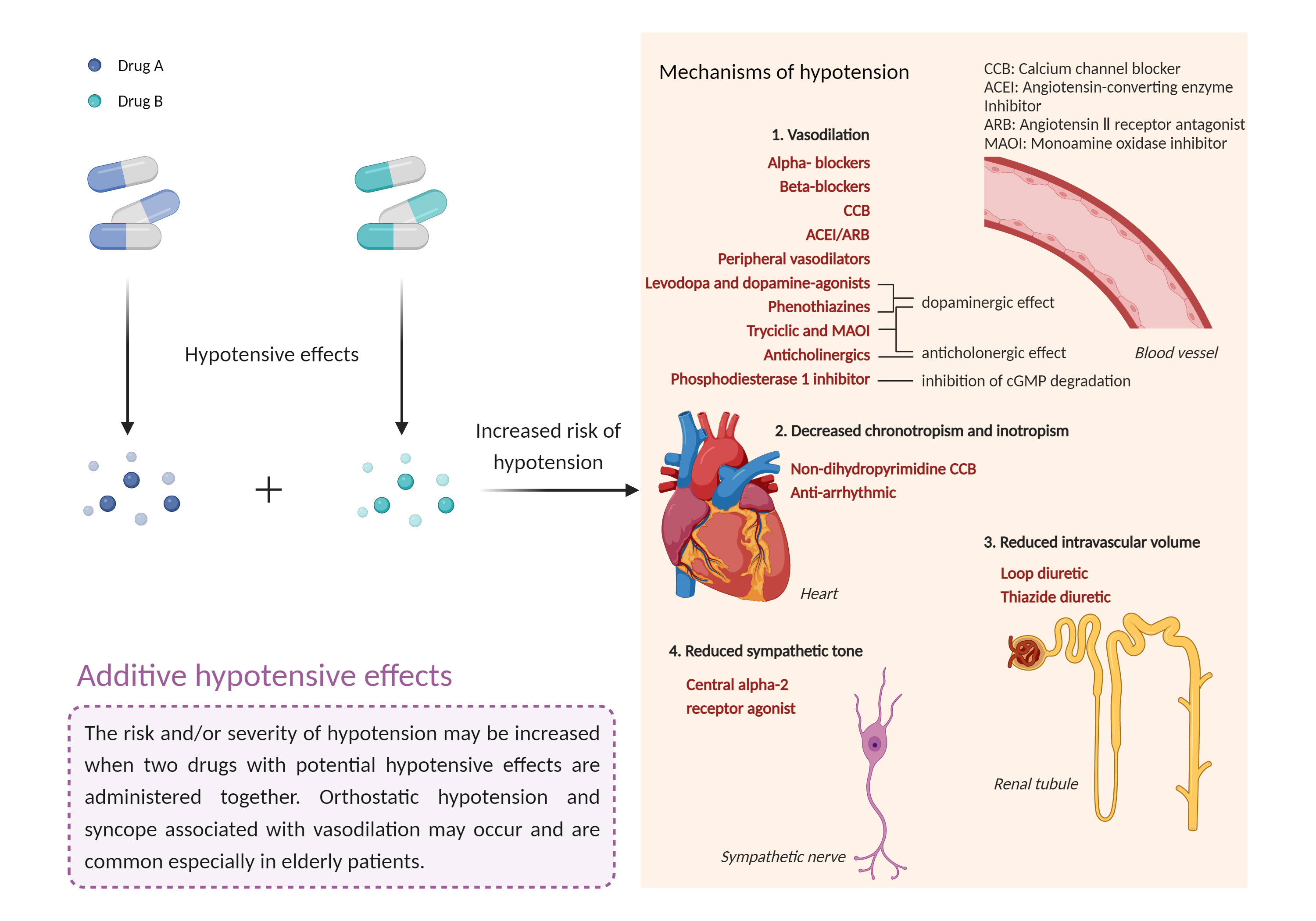
| Additive hypotensive effects Click to Show/Hide Mechanism Graph | |||||||||
 |
|||||||||
| Drug Name | Metyrosine | Canagliflozin | |||||||
| Mechanism 1 |
Antihypertensive agent Tyrosine 3-monooxygenase Binder |
Antihypertensive agent | |||||||
| Key Mechanism Factor 1 | |||||||||
| Factor Name | Tyrosine 3-monooxygenase |
×
Structure
Sequence
MPTPDATTPQAKGFRRAVSELDAKQAEAIMVRGQGAPGPSLTGSPWPGTAAPAASYTPTPRSPRFIGRRQSLIEDARKEREAAVAAAAAAVPSEPGDPLEAVAFEEKEGKAVLNLLFSPRATKPSALSRAVKVFETFEAKIHHLETRPAQRPRAGGPHLEYFVRLEVRRGDLAALLSGVRQVSEDVRSPAGPKVPWFPRKVSELDKCHHLVTKFDPDLDLDHPGFSDQVYRQRRKLIAEIAFQYRHGDPIPRVEYTAEEIATWKEVYTTLKGLYATHACGEHLEAFALLERFSGYREDNIPQLEDVSRFLKERTGFQLRPVAGLLSARDFLASLAFRVFQCTQYIRHASSPMHSPEPDCCHELLGHVPMLADRTFAQFSQDIGLASLGASDEEIEKLSTLYWFTVEFGLCKQNGEVKAYGAGLLSSYGELLHCLSEEPEIRAFDPEAAAVQPYQDQTYQSVYFVSESFSDAKDKLRSYASRIQRPFSVKFDPYTLAIDVLDSPQAVRRSLEGVQDELDTLAHALSAIG
|
|||||||
| Gene Name | TH | ||||||||
| Uniprot ID | TY3H_HUMAN | ||||||||
| KEGG Pathway | hsa:7054 | ||||||||
| Protein Family | Biopterin-dependent aromatic amino acid hydroxylase family | ||||||||
| Protein Function |
Catalyzes the conversion of L-tyrosine to L-dihydroxyphenylalanine (L-Dopa), the rate-limiting step in the biosynthesis of cathecolamines, dopamine, noradrenaline, and adrenaline. Uses tetrahydrobiopterin and molecular oxygen to convert tyrosine to L-Dopa (PubMed:17391063, PubMed:1680128, PubMed:15287903, PubMed:8528210, Ref.18, PubMed:34922205, PubMed:24753243). In addition to tyrosine, is able to catalyze the hydroxylation of phenylalanine and tryptophan with lower specificity (By similarity). Positively regulates the regression of retinal hyaloid vessels during postnatal development (By similarity).
Click to Show/Hide
|
||||||||
| Mechanism Description |
|
||||||||
| Mechanism 2 |
Antihypertensive agent Tyrosine 3-monooxygenase Binder |
Hypotensive effects | |||||||
| Key Mechanism Factor 2 | |||||||||
| Factor Name | Tyrosine 3-monooxygenase |
×
Structure
Sequence
MPTPDATTPQAKGFRRAVSELDAKQAEAIMVRGQGAPGPSLTGSPWPGTAAPAASYTPTPRSPRFIGRRQSLIEDARKEREAAVAAAAAAVPSEPGDPLEAVAFEEKEGKAVLNLLFSPRATKPSALSRAVKVFETFEAKIHHLETRPAQRPRAGGPHLEYFVRLEVRRGDLAALLSGVRQVSEDVRSPAGPKVPWFPRKVSELDKCHHLVTKFDPDLDLDHPGFSDQVYRQRRKLIAEIAFQYRHGDPIPRVEYTAEEIATWKEVYTTLKGLYATHACGEHLEAFALLERFSGYREDNIPQLEDVSRFLKERTGFQLRPVAGLLSARDFLASLAFRVFQCTQYIRHASSPMHSPEPDCCHELLGHVPMLADRTFAQFSQDIGLASLGASDEEIEKLSTLYWFTVEFGLCKQNGEVKAYGAGLLSSYGELLHCLSEEPEIRAFDPEAAAVQPYQDQTYQSVYFVSESFSDAKDKLRSYASRIQRPFSVKFDPYTLAIDVLDSPQAVRRSLEGVQDELDTLAHALSAIG
|
|||||||
| Gene Name | TH | ||||||||
| Uniprot ID | TY3H_HUMAN | ||||||||
| KEGG Pathway | hsa:7054 | ||||||||
| Protein Family | Biopterin-dependent aromatic amino acid hydroxylase family | ||||||||
| Protein Function |
Catalyzes the conversion of L-tyrosine to L-dihydroxyphenylalanine (L-Dopa), the rate-limiting step in the biosynthesis of cathecolamines, dopamine, noradrenaline, and adrenaline. Uses tetrahydrobiopterin and molecular oxygen to convert tyrosine to L-Dopa (PubMed:17391063, PubMed:1680128, PubMed:15287903, PubMed:8528210, Ref.18, PubMed:34922205, PubMed:24753243). In addition to tyrosine, is able to catalyze the hydroxylation of phenylalanine and tryptophan with lower specificity (By similarity). Positively regulates the regression of retinal hyaloid vessels during postnatal development (By similarity).
Click to Show/Hide
|
||||||||
| Mechanism Description |
|
||||||||
| Recommended Action | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Management | Caution is advised if SGLT-2 inhibitors are coadministered with diuretics and other hypotensive agents, particularly in the elderly and patients with impaired renal function. Prior to initiating SGLT-2 inhibitors, volume status should be assessed and corrected, if necessary. Clinical and laboratory monitoring are recommended during therapy, including electrolytes, fluid status, renal function, and blood pressure. If volume depletion occurs, treatment with SGLT-2 inhibitors should be interrupted until the condition is corrected. | ||||||||
