| Mechanism of Asparaginase Escherichia coli-Caplacizumab Interaction
(Severity Level: Moderate)
|
|
Increased risk of bleeding
Click to Show/Hide Mechanism Graph
|
 |
| Drug Name |
Asparaginase Escherichia coli |
Caplacizumab |
|
Mechanism
|
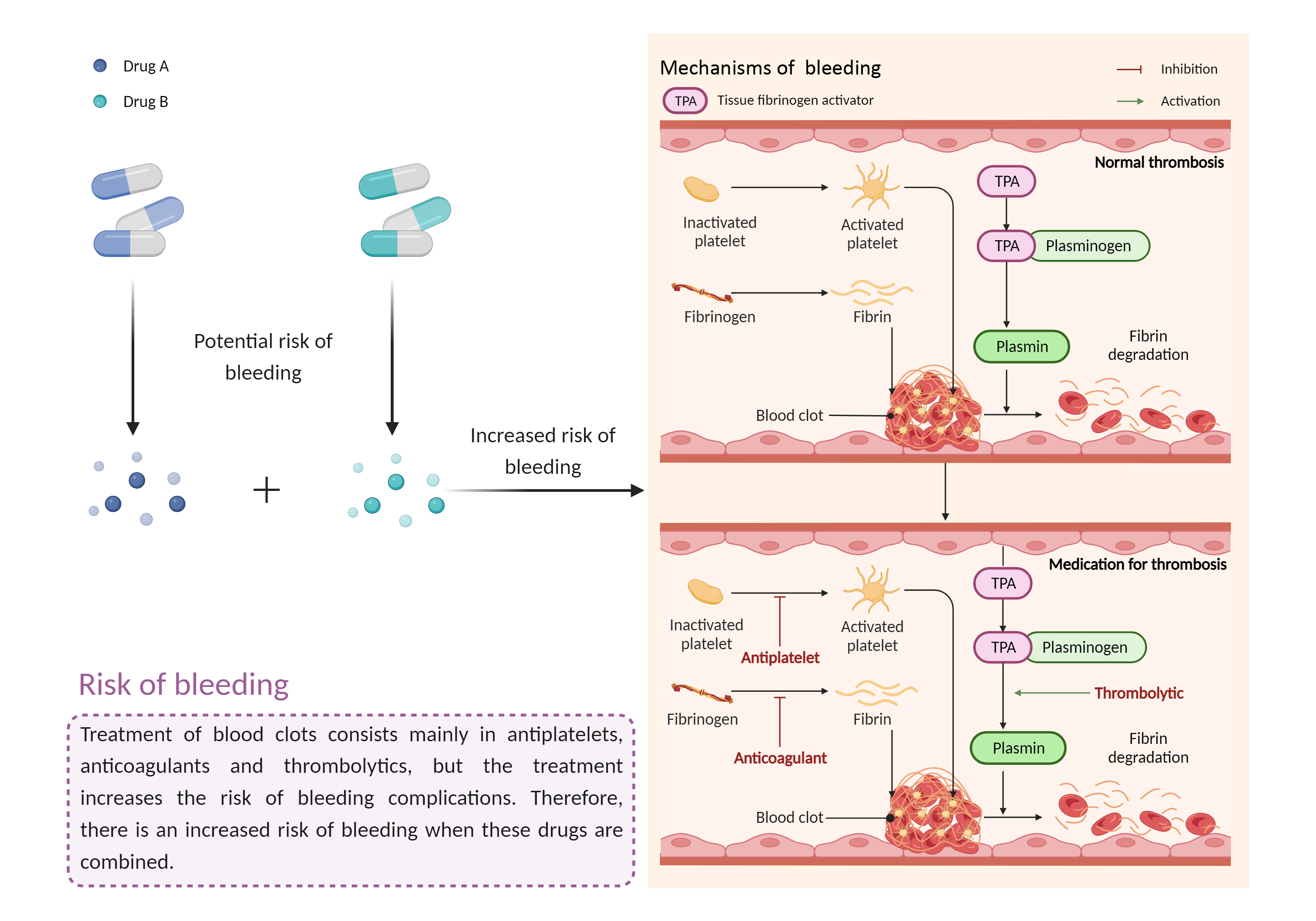
Risk of bleeding
Anticoagulant effects
|
Risk of bleeding
Antiplatelet
|
| Key Mechanism Factor 1 |
| Factor Name |
Bleeding |
| Factor Description |
Patients may be at risk for bleeding when the outcome of a disease or disease treatment confounds the standard mechanisms for maintaining hemostasis. Signs or symptoms of abnormal bleeding include: bleeding that takes a long time to stop (including nosebleeds, bleeding gums, bleeding from cuts and abrasions, and menstrual bleeding); severe unexplained bruising, or bruising that becomes larger; blood in the urine or stool, etc. |
| Mechanism Description |
- Increased risk of bleeding by the combination of Asparaginase Escherichia coli and Caplacizumab
|

